Introduction
Blood pressure is one of the most important vital signs used to assess the overall health status of an individual. It reflects the force exerted by circulating blood against the walls of the arteries and provides critical information about the functioning of the heart and blood vessels. Abnormal blood pressure levels, whether too high or too low, can be early indicators of serious medical conditions such as cardiovascular disease, stroke, kidney failure, and other life-threatening disorders.
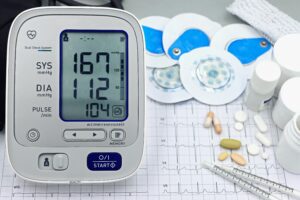
A Blood Pressure Monitor medically known as a Sphygmomanometer, is a fundamental medical device used to measure blood pressure accurately. It is widely used in hospitals, clinics, community health centers, and even in home-care settings. Due to the increasing global prevalence of hypertension, the role of blood pressure monitoring has become more important than ever.
This article provides a comprehensive and professional discussion of the Blood Pressure Monitor, covering its definition, historical development, components, types, working principles, clinical importance, correct usages, advantages, limitations, and future advancements. The information is presented in a clear, human-like academic style suitable for educational and professional purposes.
Definition of Blood Pressure Monitor (Sphygmomanometer)
A Blood Pressure Monitor is a medical instrument designed to measure the pressure of blood within the arterial system. The term sphygmomanometer is derived from Greek words: sphygmos meaning pulse, manos meaning thin or light, and metron meaning measure. Together, the term refers to a device that measures arterial pressure through pulse detection.
Blood pressure readings consist of two numerical values:
- Systolic Blood Pressure (SBP): The pressure exerted on arterial walls when the heart contracts and pumps blood.
- Diastolic Blood Pressure (DBP): The pressure in the arteries when the heart relaxes between beats.
These values are recorded in millimeters of mercury (mmHg), for example, 120/80 mmHg, which is considered a normal blood pressure reading for a healthy adult.
Historical Background
The development of blood pressure measurement dates back to the early 18th century. The first recorded blood pressure measurement was performed in 1733 by Stephen Hales, an English clergyman and scientist, who measured blood pressure in animals using invasive techniques. Although groundbreaking, his method was impractical for clinical use.
In 1896, the modern sphygmomanometer was introduced by the Italian physician Scipione Riva-Rocci, who developed a non-invasive cuff-based device. This invention marked a major milestone in medical diagnostics. Later, in 1905, Russian physician Nikolai Korotkoff discovered the Korotkoff sounds, which allowed clinicians to accurately identify systolic and diastolic pressures using a stethoscope.
Over time, technological advancements led to the development of aneroid and digital blood pressure monitors, making blood pressure measurement more accessible, accurate, and user-friendly.
Components of a Blood Pressure Monitor
A traditional sphygmomanometer consists of several essential components:
- Inflatable Cuff: Wrapped around the upper arm to temporarily restrict blood flow in the artery.
- Inflation Bulb: Used to pump air into the cuff manually.
- Pressure Gauge: Displays the pressure within the cuff, either using mercury, mechanical (aneroid), or digital readings.
- Release Valve: Controls the gradual release of air from the cuff.
- Stethoscope (for manual devices): Used to listen to Korotkoff sounds over the brachial artery.
Digital blood pressure monitors replace manual components with electronic sensors and automated systems, simplifying the measurement process.
Types of Blood Pressure Monitors
Blood pressure monitors are categorized based on their design and method of measurement:
1. Mercury Sphygmomanometer
This is the traditional and most accurate type of blood pressure monitor. It uses mercury to measure pressure and is considered the gold standard in clinical settings. However, due to environmental and safety concerns related to mercury, its use has declined.
2. Aneroid Sphygmomanometer
Aneroid devices use a mechanical gauge instead of mercury. They are portable, lightweight, and commonly used in clinics. However, they require regular calibration to maintain accuracy.
3. Digital (Electronic) Blood Pressure Monitor
Digital monitors use electronic sensors and automated cuffs to measure blood pressure. They are widely used in hospitals and home settings due to their ease of use. Measurements are displayed on a digital screen, and some models store readings for future reference.
4. Ambulatory Blood Pressure Monitor
This specialized device measures blood pressure continuously over 24 hours while the patient performs daily activities. It provides detailed data and is useful for diagnosing white-coat hypertension and masked hypertension.
Principle of Operation
The blood pressure monitor works on the principle of temporarily occluding blood flow in an artery and gradually restoring it while monitoring pressure changes. When the cuff is inflated above systolic pressure, blood flow stops completely. As the cuff pressure is slowly released, blood begins to flow through the artery, producing sounds known as Korotkoff sounds.
- The appearance of the first Korotkoff sound indicates systolic pressure.
- The disappearance of the sounds indicates diastolic pressure.
Digital devices use oscillometric methods, detecting pressure oscillations in the cuff caused by arterial blood flow and converting them into numerical values using internal algorithms.
Clinical Importance of Blood Pressure Monitoring
Blood pressure monitoring plays a critical role in modern healthcare. It is essential for:
- Diagnosis of Hypertension and Hypotension
- Monitoring cardiovascular health
- Assessing response to medications
- Preventing complications such as stroke and heart attack
- Managing chronic diseases like diabetes and kidney disorders
Regular blood pressure monitoring allows early detection of abnormalities and timely medical intervention, significantly reducing morbidity and mortality rates.
Proper Use of a Blood Pressure Monitor
Accurate blood pressure measurement requires proper technique. Key guidelines include:
- The patient should rest for at least five minutes before measurement.
- The arm should be supported at heart level.
- The cuff size must be appropriate for the arm circumference.
- The patient should avoid talking or moving during measurement.
- Multiple readings should be taken for accuracy.
Failure to follow correct procedures can lead to inaccurate readings and misdiagnosis.
Advantages of Blood Pressure Monitors
- Non-invasive and safe
- Easy to use
- Provides immediate results
- Essential for preventive healthcare
- Enables home monitoring and patient empowerment
Limitations and Challenges
Despite their benefits, blood pressure monitors have certain limitations:
- Inaccurate readings due to improper cuff size or technique
- Digital devices may be affected by movement or irregular heart rhythms
- Requires regular calibration and maintenance
Understanding these limitations helps ensure correct interpretation of results.
Future Developments
Advancements in medical technology are leading to the development of smart blood pressure monitors integrated with mobile applications, artificial intelligence, and wearable devices. These innovations aim to improve accuracy, continuous monitoring, and data sharing between patients and healthcare providers.
Conclusion
The Blood Pressure Monitor (Sphygmomanometer) is a vital medical device that plays an indispensable role in healthcare. From its historical origins to modern digital innovations, it has evolved into an essential tool for diagnosis, monitoring, and prevention of cardiovascular diseases. Accurate blood pressure measurement not only saves lives but also enhances the quality of healthcare delivery.
As the global burden of hypertension continues to rise, the importance of blood pressure monitoring cannot be overstated. Proper knowledge, correct usage, and continued technological advancements will ensure that this essential device remains a cornerstone of medical practice.